Never Be Ashamed For Being Different
Throughout my school years, I hid my diabetes from my peers. I felt embarrassed and ashamed for having a disease that was easily misunderstood. When I went to class I never came fully prepared for a low blood sugar. I wouldn’t check my blood sugar or administer insulin in front of people. If I had to attend to my diabetes, I would do so in the bathroom. The only people aware of my condition was my family (of course) and a few really close friends.
I didn’t want to be treated or viewed differently from everyone else.
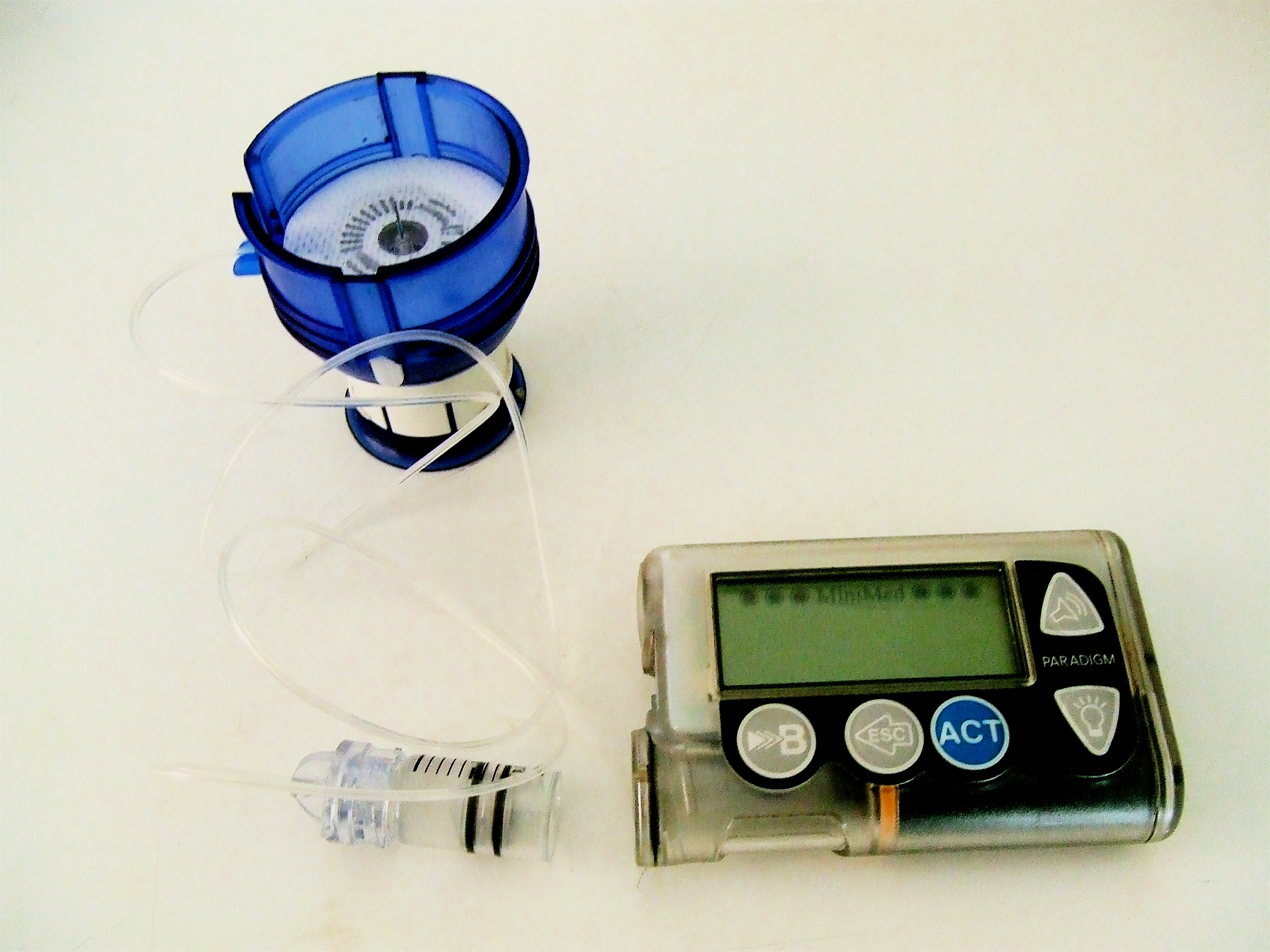
It went to such far extremes that I was putting my life at risk at times. Which ironically became even more humiliating when it came down to it. I recall my doctor advising that I should try an insulin pump — which I completely avoided. I didn’t want the looks or stares that came with wearing a device attached to me.
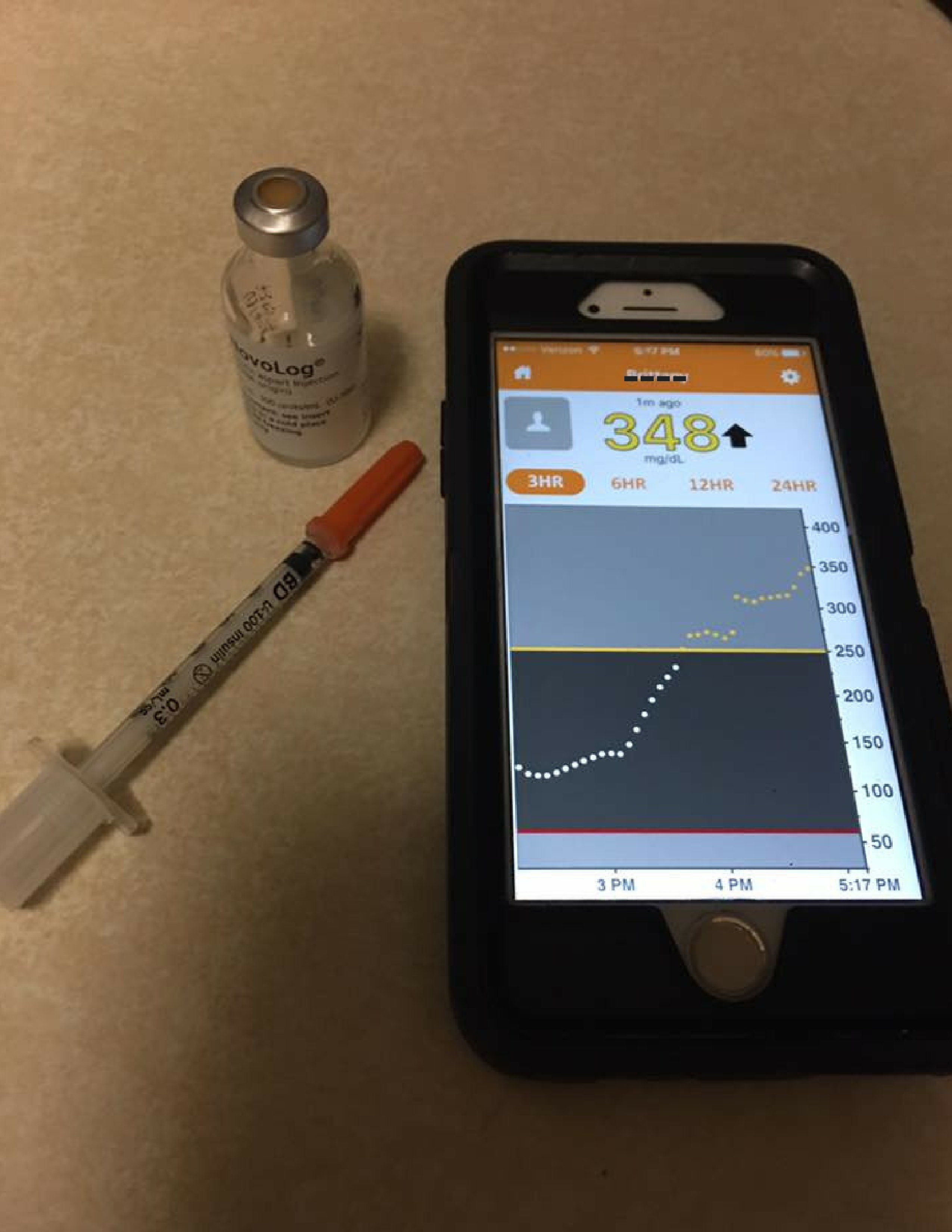
I recall getting teased on one occasion in particular at school when someone saw a insulin syringe in my purse and accused me of taking “drugs”. I simply explained: “no, this is insulin, a hormone that I MUST take everyday to stay alive.
After many years of battling my self-esteem and confidence, the worry of what other people think went away. What it eventually came down to was realizing my health and well being comes before anyone’s perception of me.
I started talking and opening up to more people about my diabetes which then brought on more conversation and ways for me to express myself. I embraced the person I’ve become by sharing what makes me different. Hiding my illness for so long made me feel like a prisoner in my own body.
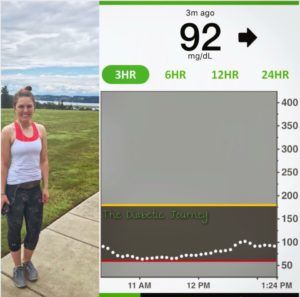
Now I have an insulin pump and CGM, which I wear proudly. I give myself insulin and check my blood sugars wherever and whenever. And in any given opportunity I try to educate more and more people because I know what it’s like to feel alone and misunderstood.
So this is my way of taking strides to inform the public and let other’s know they’re not alone. And that you should never be ashamed for being different but feel empowered for what makes you unique.